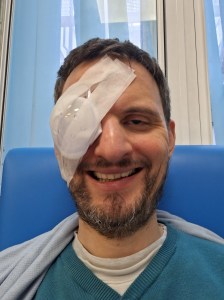
12.10am Sunday, Home: What’s gone wrong?
I was reading before going to bed when the text suddenly went blurry. “That’s very worrying,” I said out loud.
Within seconds, my right eye was only aware of the screen brightness. There was a greasy film with black dots floating around on it. My left eye was unaffected. A sense of dread descended and my pulse quickened.

I was not totally unprepared. Since birth I have had a visual impairment called aniridia. I’ve always been short-sighted, my acuity is 6/36 (typical sight is 6 times better than mine). Further sight loss was also likely at some point, not just due to old age. 9 years ago cataracts developed over a few months in both my eyes. I went from having no aids to needing a white cane and text read out to me. Operations restored my sight to the (low) level it had been previously. Compared to others with the same condition, I’d been relatively lucky with my acuity and its stability. So I have a good enough understanding of eye anatomy and my risk factors to take this seriously.
All that said, it was very scary; one eye had instantly returned to the worst period of the cataracts.
But I stayed calm and practical.
I tried my regular lubricating eye drops first, in case something was simply sitting on the surface of the eye. They made no difference.
I turned to an AI assistant. I described the above medical history and what had happened, asking it to respond as an expert ophthalmologist. The response was measured and clear. It outlined several possible causes, among them what I had guessed: retinal detachment. It advised that I should see a doctor immediately.
“What does that mean in the middle of the night at the weekend?!”
Fortunately, I live in London and have regular checkups at the world-renowned Moorfields Eye Hospital. I knew they had a 24-hour accident and emergency department. I looked up the details. I figured that the sooner any (waiting for) treatment could begin, the better, and it was likely to be quieter now than in the daytime.
I went downstairs, where my wife was watching TV. I told her what had happened and that I thought I needed to go to Moorfields right away. Equally concerned she agreed. I said there was little use her coming to wait-up with me during the early hours: she should go to bed and I’d call if and when I needed help.
1:00 Sunday: Into the dark
We prepared a bag with things to keep me going: food, reading material and an inflatable pillow!
We hugged with worry and trepidation before I set off. I took an Uber into town, passing by oblivious revellers in Stoke Newington and Hackney.
1:21am Sunday, Old Street: Unexpected challenges
The emergency department was quieter than I had expected, mostly empty with lights off. The receptionist took my details and went to speak with a clinician. She returned quickly with instructions I had not anticipated.
My symptoms pointed to an issue that was not absolutely critical. It could be investigated when the department was fully staffed. I should come back at 8am. I was given a chit to bypass triage at least.
It was now nearly 2am. I faced the prospect of getting home, sleeping and returning within six hours. I walked to 4 nearby hotels but found them all fully booked. I considered going back to snooze in a hospital chair. But I feared I’d be sitting there for many more hours later in the day too.
I made my way home and got into bed around 3.15am.
8.00am Sunday: Moorfields Eye Hospital Emergency Department
After 2½ hours of sleep and another train ride I was back at the hospital, along with many other worried people in something like the same condition as mine.
At 9.00am a nurse did the standard sight tests. My right eye could only discern the vague shape of a hand moving in front of a light.
At 11.00am I saw a doctor who did an ultrasound examination. While he could see blood in the liquid vitreous that fills the eyeball, he could not see a retinal detachment, though that had to be suspected. He referred me to the Vitreoretinal Emergency Clinic. He explained that they do examinations in the morning to prioritise their surgery in the afternoon. So if I went up right away I risked not getting dealt with today. It was best to go first thing the next day.
On my way home I noticed that I was bumping into things as I couldn’t judge distances, and was unaware of people close by on my right.
Exhausted, after lunch, I slept for the rest of the day.
8.00am Monday: Moorfields Vitreoretinal Emergency Clinic
As ever proceedings began with an acuity test. I was just about able to see a large letter held about a meter away from my right eye.
Another ultrasound again could not clearly identify the cause of the vitreous clouding, nor therefore the likely prognosis.
The doctor explained my choice.
Option 1: Watchful waiting
Do nothing and hope that over a few months the blood and cells floating in the vitreous will settle and get reabsorbed. The advantage was that there would be no risky intervention on an eye already complex due to aniridia. The disadvantage was that there was no guarantee it would clear, as the cause could continue. More seriously, if there was an underlying retinal issue, it would remain undetected and could deteriorate further without any clear warning signs. I’d have to visit the hospital regularly for checks.
Option 2: Surgery
A vitrectomy would remove the cloudy vitreous fluid and enable the surgeon to examine the retina to find, and if necessary, treat the problem. In time the eye would naturally refill it with clear fluid, restoring sight. The recovery would likely be shorter: weeks, with only one follow up visit. On the other hand, on top of the standard surgery risks, for people with aniridia, there is an elevated risk of inducing glaucoma or even aniridia fibrosis syndrome – which could reduce sight in the longer term.
Decision
I chose surgery. My level of sight was already very low. I hoped for the faster restoration and to avoid the uncertainty of both the cause being a one-off or ongoing and whether it would be improving or worsening over time. That it was even offered reassured me that surgery was worthwhile. That was my personal calculation, and it will not be the right one for everyone.
10.00am Monday, London: Me, myself and eye
Surgery was not until the afternoon, so I had 3 hours to fill. I tried to visit one of the nearby museums, only to discover that they were all shut on Mondays! I eventually went to UCL where the preserved body of philosopher Jeremy Bentham is on display. After the treat of a burrito for lunch, I made my way back to the hospital.
1.00pm Monday, Operating Theatre: Making light of it
I was actually first on the list for surgery.
It was performed under local anaesthetic. Having previously had cataract operations under general anaesthetic, I was apprehensive about this. I did not relish the idea of seeing someone come at my eye with a scalpel. In practice, the worst part was the preparation: the anaesthetic injections and doing whatever they do to keep the eye open. I try not to think too much about that or the operation itself, let alone Google it!
Once underway, there was no discomfort. My left eye was shut/under a plastic cover. My right eye was too clouded to make out what was happening.
What I could perceive was both strange and fascinating: the silhouette of a long thin device akin to a vacuum’s crevice attachment. I watched it suck out the cloudy vitreous and black floaters. Next it injected a dye (akin to seeing food colouring being added to water) to help the surgeon identify bits that still need to be removed. Then it hoovered up the dye again. At other times it was a bit like looking through a kaleidoscope.
There was a trainee observing and asking questions. So I heard the surgeon explaining what they were doing. I already knew or had just read up enough to follow along and get the idea that it was positive.
They found a vasoproliferative lesion (abnormal blood vessels on the retina) which had bled. They chose to leave it alone rather than risk fiddling with it. Critically, there was no retinal detachment. They refilled the eyeball temporarily with saline and an air bubble (not a longer-lasting gas). There was also no need to maintain a specific posture (such as face down) during weeks of recovery. On the spectrum of possible causes and outcomes, this was all at the less serious end.
The procedure had taken approximately twenty minutes.
Soon, they were sealing the incisions and taping on a patch. I sat up on the operating table to get into a wheelchair and be taken to recovery.
I was given a cup of tea and custard cream biscuits – oh, and medication for the coming weeks. I was declared unfit for work for 2 weeks. Within an hour I was free to go. I walked out, got in a taxi and was home by 4pm.
Tuesday, Home: Not a patch on normality
As instructed, I removed the eyepatch and cleaned the eye with cooled boiled water. It was bloodshot and sore. I took paracetamol for the aching. I had two types of eye drops to take 4 times a day to reduce inflammation and prevent infection.
Sight was still extremely limited, similar to before the operation. What was different was the rough black line across the middle of my vision. This was the boundary between the air bubble and saline. As I shook my head I could see it sloshing around. As advised, over the next few days the bubble got smaller as the air dissipated to be replaced by natural fluid.

Counterintuitively, the line descended rather than rose in my field of view. I tried in vain to understand why. I believe this paper explains it: Optical Effects of Intraocular Gas Tamponade.
An AI assistant explained it in this simplified way:
“The lens inverts the image projected onto the retina — light from above hits the lower retina, light from below hits the upper retina. As the air bubble shrank, its lower boundary rose inside the eye, unblocking the upper retina first. Since the brain corrects for the lens inversion, this appears as the line moving downward in perceived vision.”
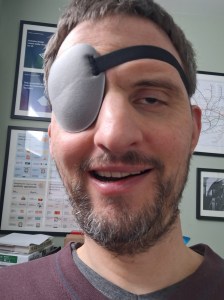
The jiggling line was quite distracting; it made me feel a bit motion sick. The blurriness interfered with the sight of my left eye. I got a patch to reduce the effect of both.
Thursday, Home: Keeping my spirits up
3 days later, the air bubble formed an arc when looking forward and a circle when looking at the floor. I could jiggle it around. It continued getting smaller. It was like looking through a spirit level. If other surgical gases had been necessary the bubble would have lasted weeks.

Meanwhile my vision slowly began to get clearer. While it lasted, the bubble actually was the best area and even had a slightly magnifying effect.
I found brightness difficult as it was scattered by the blurriness to become glare. I could see backlit screens, but white backgrounds overwhelmed black text.
I found that switching my computer and phone to dark mode (white text on a dark background) helped significantly. Very encouraging.
Friday, Home: Words of encouragement
4 days after surgery, my right eye could read text on my phone again. It was difficult, like looking through a condensation-covered window, but readable. That felt wonderful.

Tuesday, Vitreoretinal Emergency Clinic: Bubble busted
Over the weekend the bubble had shrunk to be a circle, only visible with my neck bent to look at the floor. It then disappeared.
However, I was experiencing really bad headaches/pain. I had thought they were due to the surgery or disorientation. But that had passed while the ache around my right eye had grown. It kept me awake at night and incapacitated me the following day – though paracetamol helped a lot.
After phoning for advice, I returned to the Vitreoretinal Emergency Clinic.
As I suspected, the pressure in my right eye was high (30 mmHg), compared to my left eye (20 mmHg) and my normal readings.
My medication was changed:
- fewer dexamethasone drops (anti-inflammatory steroids) that can cause pressure to rise.
- new anti-inflammatory and pain relief, non-steroidial drops (Acular – Ketorolac Trometamol)
- drops to reduce the production of fluid in the eye to reduce the pressure (Cosopt/Codimaz – Dorzolamide/Timolol).
Sunday: Working well
Two weeks after the bleed and surgery, my vision is almost back to normal (for me) -I think. The main difference between the vision in each eye is that the right has a yellow tint. It is more sensitive to bright light but I think it always was the one I’d squint most anyway. Hopefully, the tint will reduce as the fluid clears further.
I’m due to return to work. I have a follow-up appointment at Moorfields in a few days.
Reflections
One thing I found difficult during recovery was the lack of illustrations of the experience to compare to my own. That’s partly why I wrote this post.
One account suggested that the bubble area should be relatively clear. I was worried at first that was not the case for me.
The sudden loss of functional vision is frightening. I tried to take each step at a time, noting that I still had a half-decent eye and that I had a lot of great support around me, at home, at work and in hospital to deal with the problem however it turned out.
The care I received at Moorfields was excellent and amazingly fast. From the moment the bleed occurred, until surgery was about 37 hours. Then nearly completely vision restoration within a fortnight.
I feel some things should be better though. They have not had an impact on me but I can see how they could on other people.
- When I looked it up, the emergency phone line for Moorfields A&E was not 24 hours or even 7 days a week. One call would have avoided my early hours dash to central London. Perhaps it could have diverted to NHS 111.
- The hospital could have offered me a comfortable place to sleep between 2am and 7am rather than sending me away.
- I’d like the medical staff to indicate they have looked at my extensive eye health notes before speaking to me. Because I couldn’t be sure they had all the information, I felt I needed to explain facts such as my underlying aniridia and prior cataract operations. It was unnerving.
Thank you
I want to thank everyone at Moorfields Eye Hospital who was involved in my care. I am grateful also to my regular ophthalmologists, who were supportive when I informed them by email.
Most of all, I want to thank my wife. She sent me off into the night with composure and kindness when it was very concerning for her too. She has been wonderful and patient with the patient throughout.
If similar has happened to you
Sudden vision loss needs to be assessed urgently. Get in front of an eye doctor as quickly as you can.
Consider the options of waiting and surgery in advance if you can. If you are facing the same decision, talk it through honestly with your surgeon. There is no universally right answer. The choice depends on your eyes, thoughts on surgery, circumstances, and what you can live with.
For those with aniridia or other pre-existing conditions, the additional surgical risks are worth discussing specifically, not dismissing.
My very best wishes for a swift and successful recovery to you.